A new, more convenient method of detecting breast cancer has begun testing in the United Kingdom, with the potential to identify tumors at an earlier stage.
At some time in their life, one in every eight British women will be diagnosed with breast cancer. Because malignancies and fibrous tissue both show up as solid white regions on X-ray, mammograms are less effective in younger women whose breasts contain denser, fibrous tissue and less fat because cancers and fibrous tissue both appear as solid white areas on X-ray.
Mammograms may miss malignancies in postmenopausal women with thick breast tissue, who are also more likely to acquire breast cancer in the first place.
Women with a dubious lump may be given an ultrasound scan or a biopsy, and if the diagnosis is still unclear, they may be directed for DCE-MRI, which detects the development of new blood vessels supporting tumors. However, in women with early-stage malignancies, they may not be visible, leading to false comfort.
Multiparametric MRI was first created to evaluate liver disorders without the need for a painful biopsy, and it is now widely utilized in Europe and the United States.
It works similarly to traditional MRI in that it utilizes high magnetic fields and radio waves to excite protons in the tissue, then exploits variations in the time it takes for them to settle to generate a “map” of the various tissues in the breast. Multiparametric MRI, on the other hand, allows an even more comprehensive map to be generated by merging pictures created by multiple MR pulses and sequences.
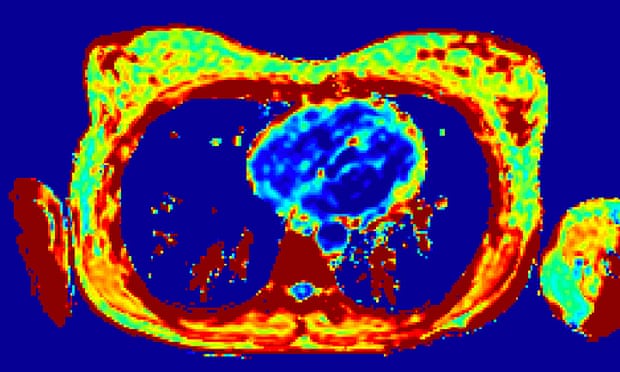
“We believe that if we differentiate the tissue rather than looking at the blood vessels around the tumor, we should be able to spot not only tumors in dense breasts but potentially tumors that aren’t seen on mammograms,” said Prof Sally Collins, a consultant obstetrician and medical lead for women’s health at Oxford-based Perspectum Diagnostics, who herself recently received treatment for breast cancer.
“We’re also working to improve the scanning experience for patients. “Mammograms are awful because they squish your breast on this plate, which is undignified and unpleasant, and MRIs are much worse because you have to lie face down with your boobs dangling in this coil and your arms raised over your head for ages,” Collins added.
“We’re attempting to make it such that women may be fully dressed, respectable, and comfortable while being scanned, which is critical for the patient journey to cancer diagnosis.”
The prospectus has received ethical clearance to enroll 1,030 women in the study, including 10 women who have been diagnosed with breast cancer and 30 to 40 healthy women who are presently being scanned, to see if the technology can properly map their breast tissue while laying on their backs. It is estimated that the study would take two years to complete.
“It will never replace regular mammography screening for postmenopausal women, but we think it will enhance the diagnosis route for women with thick breasts or premenopausal women who are at extremely high risk of breast cancer, eliminating the need for repeated tests,” Collins said.


You must be logged in to post a comment.