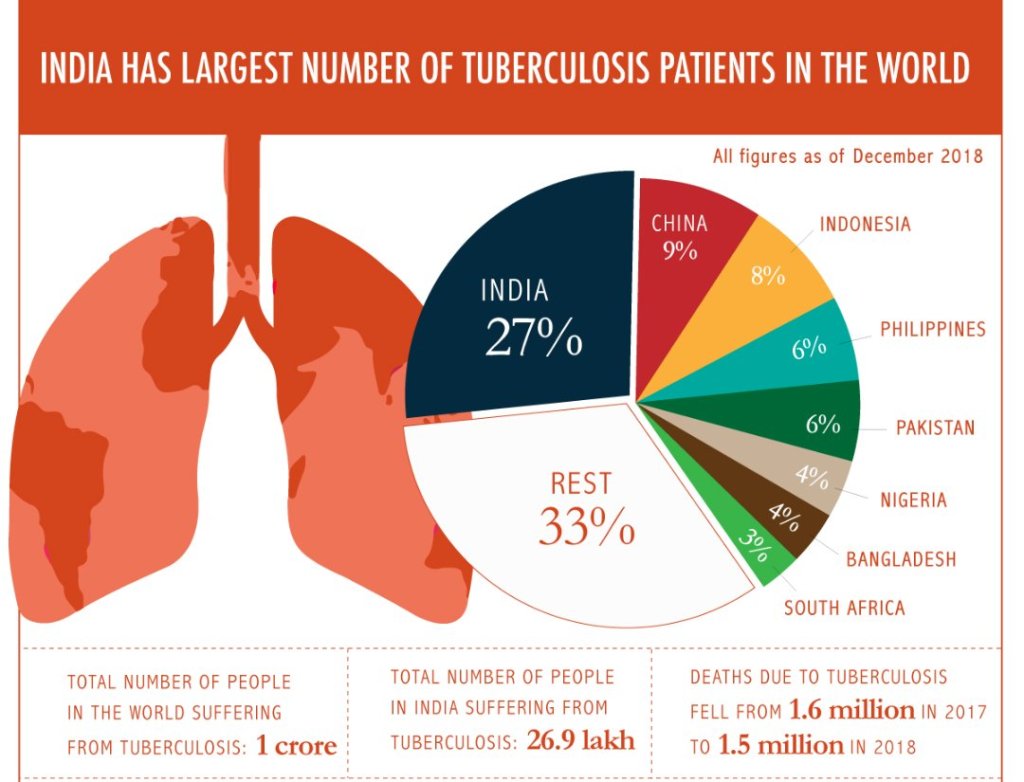
Tuberculosis is a pandemic globally become significant health threat in many countries. India top the list of having most tuberculosis patients. TB is airborne disease. Every year, India estimated TB patient is 28 lakhs, which is 27 per cent of the global total, almost 1200 TB patient die everyday, 10 every 3 minutes. In 2017, 204 TB cases per 1,00,000 encountered. India has the highest number of multi drug resistant TB (MDR-TB) cases in the world. Largest number of people living with multi resistance TB which normal dosage of Isoniziad and INH will not work on patient or first line drug of TB will not work on you.
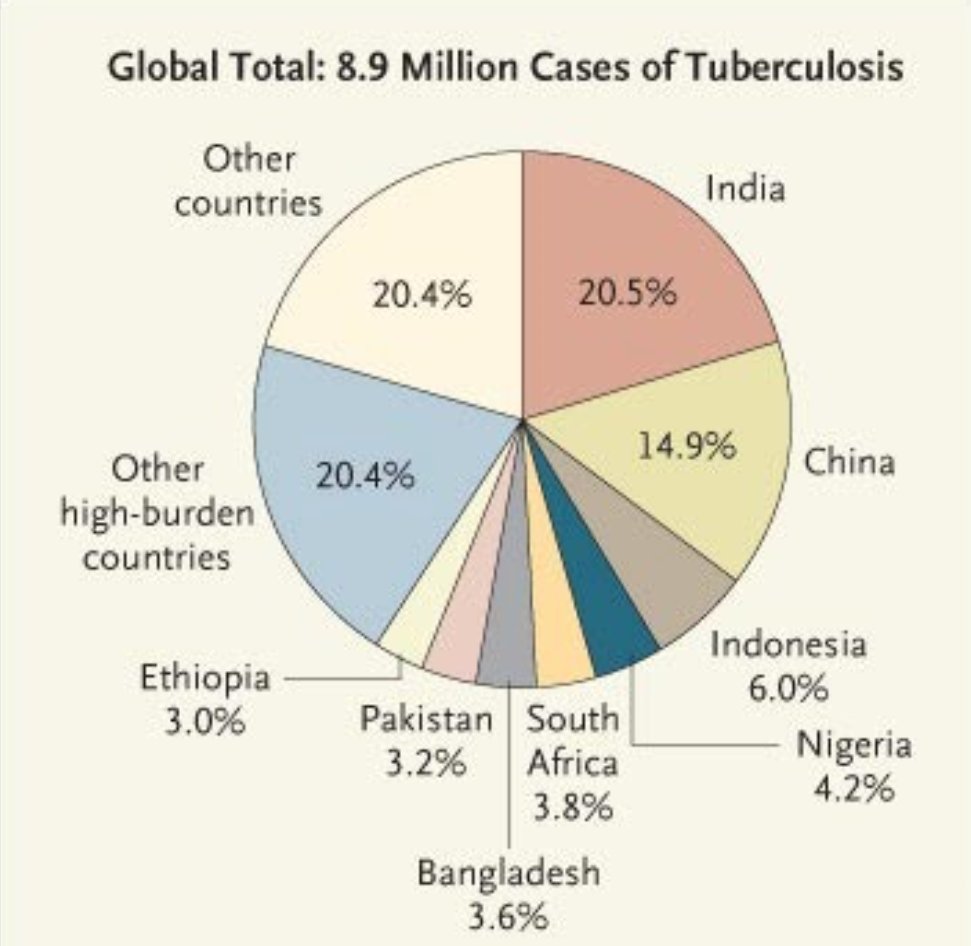
According to Health Ministry & Welfare data explain, only 63 per cent of the patients infected with airborne disease and currently under treatment. Further, 1,47,000 patients are resistant to first and second line TB medicines. World Health Organization (WHO) reported India had 2.7 million new cases and 440,000 deaths due to TB in 2018 – the highest in the world. Despite such conditions India has not implemented goal measures effectively to control the spread of TB. Imagine if we are not capable to control TB then can we measure Coronavirus? when we have paucity of hospital, less number of health workers and doctors.
HISTORY OF TUBERCULOSIS IN INDIA

For TB patients first open air isolation institution and treatment of TB patients was started in Ajmer & almore 1906. The anti TB movement in the country gained momentum with TB association of India which was established in 1939.
The Bhore committee report issued in 1946 estimated that about 2.5 million patients required treatment in the country with 6,000 beds available. National Tuberculosis Control programme (NTP) was formulated in 1962. NTP was not implemented properly then revised into National TB Control Programme (RNTCP) was developed. Sir Joseph Bhore recommended re – modelling the health services integrate curative & preventive medicine at all levels. Bhore committee was not able to reach the plan , recognizing the lack of access to basic healthcare in rural areas, National Health Policy 1993 emphasized on primary care, commitment to provide “Health to all” by the year 2000. By 2000 India still not achieved most of the goals of the national health policy.
National Health Policy by 2010 & to increase public investment from 0.9% to between 20% which is 3% of GDP. National Rural Health Mission 2005 – 2012 was launched to provide Healthcare to rural population. Special focus on 18 states who has weak Healthcare system.
MEASURES TAKEN BY GOVERNMENT
Indian government launched the TB free India campaign, Target of elimination of TB in the country by 2025. DOTS – Directory observed Treatment ,it is a strategy to diagnose the TB through sputum testing.
CBNAAT – Catridge based Nuclei acid amplification test, this test help two ways to detect TB that whether person diagnose with TB, if it is TB is it MDR or the other one first line drug. First time central TB Division (CTD) introduced a quarterly ranking of TB elimination efforts by all the states and UTs. TB preventive Therepy (TPT) give financial expenditure which include in the assessment. Saksham project provide psycho – social counseling to TB patients.
Nikshay poshan yojana (NPY) scheme made to give financial support to TB patients for their nutritional diet. The Nikshay Ecosystem is the National TB information System which is one – stop solution to collected information of patients and manage program activity & evaluate through out the country.TB Harega Desh Jeetega – This strategy launched in September 2019 for fight against TB.
ARE GOVERNMENT MEASURES GOING WELL ON GROUND LEVEL
After implementing most of the best policies are not capable to eliminate TB. India known for the fact that “poor quality of Healthcare”. There is shortage of testing centres, DOT centres, and other facilities to identify and treatment of new TB patients. GOI has set a target of zero – tuberculosis deaths by the 2025 rather should focus on zero – tuberculosis patients till 2030.
Despite all the notable measures taken by the government still needs to robust efforts to improve the early diagnose for the appropriate treatment which is significant for ending of TB. We need to expand both laboratory network as well as diagnostic facilities to cover the whole nation under the umbrella of one program National TB Elimination Programme. Private sector plays crucial role in terms of providing mandatory tuberculosis treatment quality care.
The UN sustainable development Goals (SDGs) include ending the TB epidemic by 2030 under the Goal 3. India set target to eliminate TB by 2025 ( which is five years ahead of SDGs) appears ‘unrealistic’ , ‘unattainable’ as seeing today’s condition of India which requires high quality of care to each person. We need to increase TB services for those who are not able to reach the TB centres , increase the engagement of private sector facilities and support system of universal access to drug susceptibility testing and second line TB drugs.
GOI said that new tools resulting from greater tuberculosis research & development (R&D) which is important to prevent Economic losses. 30 per cent of Indian population infected with tuberculosis. Consequently, we need accurate level of care which helps for detecting tuberculosis infection. India need close coordination between Ministry of Science & Technology , Ministry of Health and Research oriented pharmaceutical companies together to reach target to fight against the Tuberculosis. India strictly implement the strategy of finding the TB cases rather waiting for patient with TB to reach to the hospital.Under the make in India program, development of a first line anti – TB drug was proposed in public sector.
Awareness about TB and its prevention among masses is important. Media campaigns must planned under the program to promote TB preventive measures swasth E – gurukul is one such initiative of WHO.
Union Health Minister , Harsh Vardhan said:
“we as a nation, need to come together to fight against tuberculosis and the stigma surrounding it so that every TB patient seek care with dignity and without discrimination. The community must act as a well spring of support and comfort for a patient”.
Union Health Minister Harshvardhan in press conference talking about social stigma around TB;
We must talk about the social stigma attach with Tuberculosis. Association of HIV with TB estimated 9 per cent of all HIV – TB deaths in the world, the second highest number globally 92,000 HIV – TB patients were accounted on annual basis.
If GOI implement all policies wisely and evaluate them in every 6 months we can reach to attain our goal to eliminate Tuberculosis from India. In rural areas, officers must help to detect TB before it become MDR by making reports of how many people each month diagnose with TB. If we do not take serious measures now it will be difficult to achieve the set target of “elimination of TB in 2025”.


You must be logged in to post a comment.